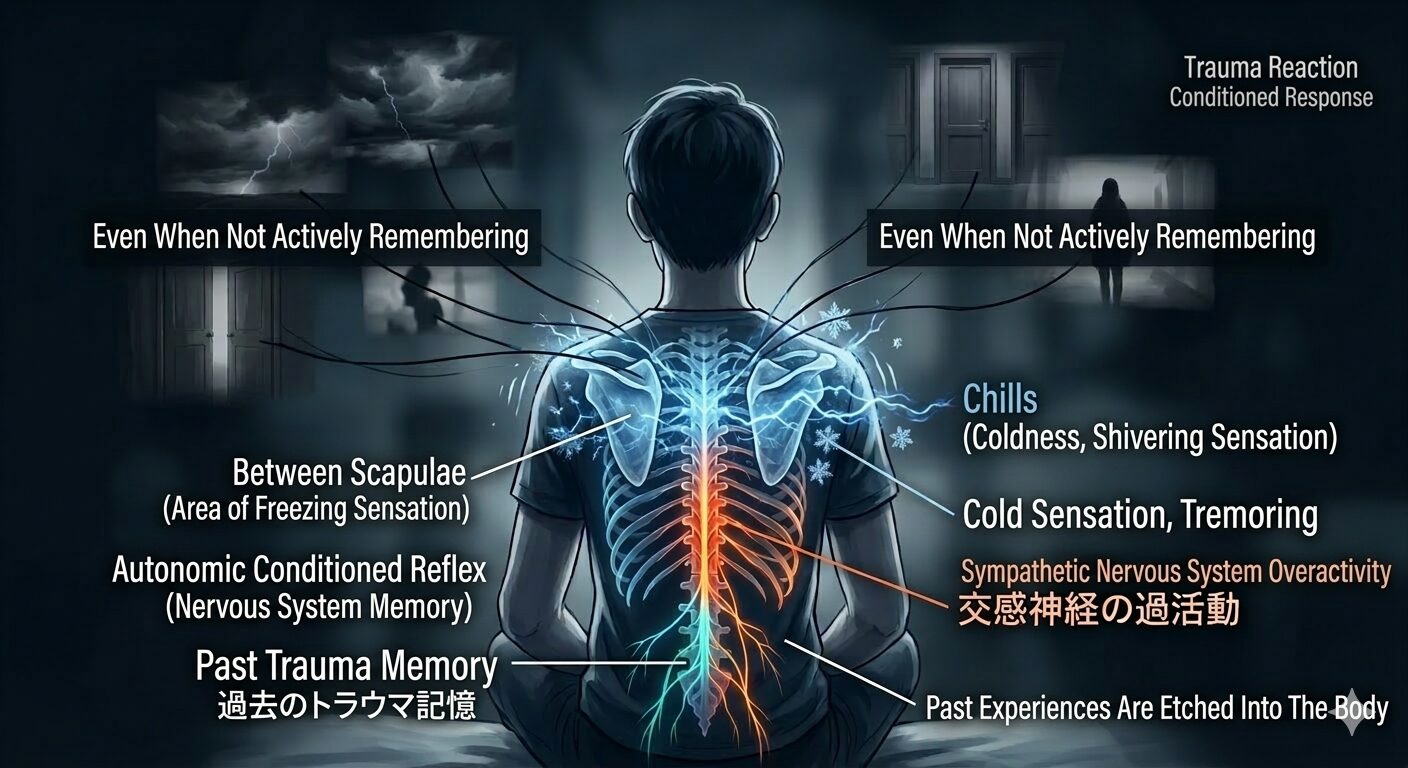
Past Stress Experience &
Abnormal Back SensationsAn Integrative Research Report on the Autonomic Nervous System and Body Memory
The chills, tremors, and “crawling” sensations between the shoulder blades are not a sign that the body is broken — they are an “echo” of a defense system that once protected you. This report systematically deconstructs and analyzes this phenomenon, from its physiological mechanisms to concrete recovery interventions.
- The Physiological Mechanisms BehindBack Chills and Abnormal Sensations
- An Anatomical Perspective: Why Symptoms AppearBetween the Shoulder Blades
- The Neuroscientific Relationship BetweenStress Memory and Bodily Response
- Somatic Approaches: Practical Interventionsto Reduce Chills and Abnormal Sensations
- Long-Term Strategies & Daily Habitsfor Autonomic Nervous System Stabilization
- Conclusion: From the Echo of the Body’sDefense System, Toward Warmth
The Physiological Mechanisms BehindBack Chills and Abnormal Sensations
The chills and abnormal sensations that arise specifically around the shoulder blades are explained by state transitions in the autonomic nervous system and the accompanying changes in peripheral circulation. When a stress response is triggered, the body performs sophisticated resource allocation to prioritize survival — and this process becomes a source of the distinctive sensations felt in the upper back.
1.1 Vasoconstriction and Peripheral Blood Flow Redistribution
When acute or chronic stress is perceived, the hypothalamus immediately activates the sympathetic nervous system, releasing epinephrine (adrenaline) and norepinephrine into the bloodstream via the sympathetic-adrenal medullary (SAM) axis. These catecholamines induce rapid vasoconstriction in blood vessels throughout the body.
The primary purpose of this physiological response is to restrict blood flow to areas not directly essential for survival — such as the skin and digestive tract — and to prioritize blood delivery to the brain, heart, and large skeletal muscles. As peripheral vessels near the skin surface constrict, skin temperature drops, and this is perceived by the central nervous system as “chills.”
Cold Sensation via Vasoconstriction
Catecholamine release from the SAM axis causes peripheral vasoconstriction. The resulting drop in skin temperature is perceived as “chills.” The upper back, densely packed with respiratory and postural muscles, is particularly prone to pronounced coldness and numbness.
Piloerection (Goosebump Response)
Sympathetic stimulation contracts the arrector pili muscles — the source of the “crawling” sensation. When the amygdala misidentifies subtle stimuli as “threats” via faulty neuroception, this reflex fires without engaging any conscious thought process.
Freeze Response & Thermal Perception
Immobilization (freeze) via the dorsal vagal pathway drives metabolism to its lowest limit. The drop in heart rate and blood pressure, combined with suppressed thermoregulation, produces generalized or localized coldness throughout the body.
1.2 Autonomic State vs. Sensory Characteristics
| ANS State | Primary Pathway | Key Physiological Changes | Sensory Characteristics |
|---|---|---|---|
| Ventral Vagal (Safety) | Myelinated vagus nerve | Stable heart rate, improved digestion, muscle relaxation | Warmth, relaxation |
| Sympathetic (Fight or Flight) | SAM axis / HPA axis | Vasoconstriction, piloerection, elevated heart rate & breathing | Crawling sensations, tremors, partial coldness |
| Dorsal Vagal (Freeze) | Unmyelinated vagus nerve | Metabolic slowing, blood pressure drop, dissociation, loss of muscle tone | Deep cold, numbness, sensory loss |
Back chills most commonly arise in a mixed state — one in which excessive sympathetic mobilization and dorsal vagal shutdown coexist simultaneously.
An Anatomical Perspective: Why Symptoms AppearBetween the Shoulder Blades
The interscapular region — the area between the shoulder blades — is a structurally and neurologically vulnerable zone where stress responses are particularly prone to somatization.
2.1 Muscular Armoring via Chronic Tension
In mammals, including humans, the back serves as an instinctive defensive line protecting the spinal cord from attack. Individuals who have experienced trauma unconsciously tense the muscles around the shoulder blades in preparation for future impacts from behind. Reichian psychology calls this Armoring.
The rhomboids, trapezius, and levator scapulae in particular are overused during the shoulder-hunching and defensive posturing that accompany stress. When these muscles remain chronically tense, the fascia adheres, compressing the cutaneous nerves and blood vessels running beneath.
2.2 Notalgia Paresthetica and Nerve Entrapment
Notalgia Paresthetica is a sensory neuropathy in which itching, chills, and abnormal sensations are confined to the region between the shoulder blades and spine. It results from entrapment of the posterior rami of thoracic spinal nerves T2–T6 by the back muscles and fascia. Psychological stress is known to heighten the sensitivity of these nerves, exacerbating symptoms.
2.3 The Spinal Accessory Nerve and Stress Response
The accessory nerve (Cranial Nerve XI) innervates the trapezius and sternocleidomastoid muscles and is exquisitely sensitive to emotional stress. The involuntary stiffening of the shoulders under stress occurs because the accessory nerve receives signals from the amygdala and commands these muscles to contract. Chronic tension at this site can persist for years as “stiffness” and “coldness” in the shoulder blade region.
The body is more honest than language.
Even without conscious memory, the muscles remember.
The Neuroscientific Relationship BetweenStress Memory and Bodily Response
The reason bodily responses arise even when “nothing is being remembered” lies in the dual structure of how memory is processed and stored within the brain.
3.1 The Divergence of Explicit Memory (Hippocampus) and Implicit Memory (Amygdala)
Under intense stress, the massive cortisol surge suppresses hippocampal function while the amygdala enters a hyperactive state. As a result, even as the specific content of an event is forgotten, the “fear, sensations, and bodily tension” of that moment are preserved in the brain without context. This is the essence of body memory.
Subtle stimuli in the present environment — a specific smell, sound, visual pattern, or even a change in one’s own heartbeat — act as triggers. The amygdala instantly sends a “danger” signal to the body. This is the direct neurological process behind the crawling back sensation that arises even without conscious recollection.
3.2 Neuroception: Threat-Scanning Below Consciousness
Neuroception, as proposed by Dr. Stephen Porges, refers to the nervous system’s ability to evaluate environmental safety far faster than conscious thought can form the judgment “this is dangerous.” In a post-trauma nervous system, neuroception is hypersensitive — or miscalibrated. Even in objectively safe situations, the brain’s deeper regions seek out “unresolved fragments of the past” and instantly activate the sympathetic nervous system. Because conscious thought (cortex) is not involved in this process, the body alone trembles or feels chills even when “nothing is being remembered.”
3.3 The HPA Axis Feedback Loop
| Hormone / Site | Behavior Under Stress | Long-Term Impact |
|---|---|---|
| CRH (Hypothalamus) | Increased release stimulates the pituitary | Heightened anxiety sensitivity, amygdala sensitization |
| ACTH (Pituitary) | Stimulates adrenal glands to release cortisol | Autonomic nervous system destabilization |
| Cortisol (Adrenal Glands) | Anti-inflammatory, blood glucose elevation, hippocampal suppression | Reduced receptor sensitivity, hippocampal atrophy |
| Amygdala | Activates and further drives the HPA axis | Stress responses triggered by minimal stimuli |
Somatic Approaches: Practical Interventionsto Reduce Chills and Abnormal Sensations
Resolving trauma responses stored in the body — incomplete survival responses — requires not only verbal understanding but also somatic regulation through a bottom-up approach: working through the body itself.
4.1 Somatic Experiencing (SE) Techniques
Pendulation
Core SE Technique — Nervous System Recalibration- 1
Direct your awareness to the uncomfortable area — the chills or crawling sensation between the shoulder blades. Rate the intensity of the sensation from 1 to 10.
- 2
Shift your awareness to an area of the body that feels relatively calm or comfortable — the contact of your feet with the floor, the warmth of your hands, and so on.
- 3
Alternate your awareness between the uncomfortable and comfortable areas. Through this, the nervous system relearns its ability to return to safety.
- 4
If the body begins to tremble naturally, or a deep sigh or yawn arises, do not suppress it — allow it to complete naturally. These are healthy signs of the autonomic nervous system discharging excess energy.
4.2 Physical Release of Fascia and Nerves
Wall Angels
Activating Rhomboids & Trapezius — Correcting Defensive Posture- 1
Stand with your back flat against a wall, ensuring four points of contact: the back of the head, shoulder blades, lower back, and heels.
- 2
Bend both arms to 90 degrees (W-shape) against the wall, then slowly slide them upward along the wall into a Y-shape overhead.
- 3
Repeat 5–10 times. Focus on the sensation of the shoulder blades drawing toward the center of your back.
4.3 Stanley Rosenberg’s Vagus Nerve Reset
Basic Exercise (Ocular Movement Method)
Activating the Ventral Vagal System — Restoring a Sense of Safety- 1
Lie on your back and interlace your fingers, placing them beneath the base of your skull (occiput).
- 2
Keeping your face directed toward the ceiling, slowly move only your eyes (eyeballs) as far to the right as they will go.
- 3
Hold this position until a spontaneous yawn, swallow, or deep sigh occurs — typically 30–60 seconds. This is the sign that the vagus nerve has reset.
- 4
Repeat on the opposite side (eyes to the left).
Long-Term Strategies & Daily Habitsfor Autonomic Nervous System Stabilization
5.1 Improving Heart Rate Variability (HRV) & Coherence Breathing
Heart Rate Variability (HRV) is a key indicator of autonomic nervous system resilience — the higher the HRV, the greater the capacity to recover from stress. Coherence breathing — approximately 6 breaths per minute (5 seconds in, 5 seconds out) — promotes synchronization between the heart and brain and suppresses sympathetic overdrive. Splashing cold water on the face in the morning, or briefly cooling the back of the neck, also trains the vagus nerve and raises overall nervous system tone.
5.2 Grounding and Orientation
When the body begins to be pulled back into the “past,” these techniques forcibly anchor awareness to the present moment.
5-4-3-2-1 Method: Sequentially identify 5 things you can see, 4 sounds you can hear, 3 textures you can touch, 2 things you can smell, and 1 thing you can taste. Consciously attending to the sensation of your feet firmly contacting the ground is also highly effective.
5.3 Utilizing Co-Regulation
In Polyvagal Theory, safe connection with another person is the single most powerful factor in stabilizing the autonomic nervous system. Conversation with a trusted person, the gentle exchange of facial expressions, or interaction with a pet instantly activates the ventral vagal system. When self-regulation proves difficult, EMDR (Eye Movement Desensitization and Reprocessing), somatic psychotherapy, or trauma-specialized counseling is strongly recommended.
Conclusion: From the Echo of the Body’sDefense System, Toward Warmth
The Nature of the Sensation: The chills and abnormal sensations in the back are an “echo” of a defense system that once protected you. The body is not broken — it is evidence of a highly sophisticated (but now unnecessary) defense system still running.
Why the Body Responds Without Remembering: Context-free body memories are stored in the amygdala, and via miscalibrated neuroception, subtle present-day stimuli reactivate past threat signals. Conscious thought (the cortex) plays no role in this process.
The Key to Recovery: The path forward lies in the body reacquiring, from the bottom up, the conviction that “right now, I am safe.” By incorporating physical stretches, vagus nerve exercises, and breathing practices into daily life, the nervous system’s hypersensitivity gradually quiets.
Professional Support: Bottom-up approaches such as SE, EMDR, and somatic psychotherapy enable neural-level recalibration that verbal understanding alone cannot reach. When self-regulation proves difficult, connecting with a professional without hesitation is essential.
The energy stored in the back as “chills” will eventually integrate into a quiet warmth. It is the hope of this report that the knowledge detailed herein will serve as one step toward recovering the nervous system’s capacity for self-regulation, and reclaiming peace of mind and body.
References & Citations
- Yokosuka Osteopathic Clinic — ANS Dysregulation & Polyvagal Theory
https://yokosuka-seikotsuin.com/blog/ - Here Counseling — Emotional Somatic Flashbacks
https://herecounseling.com/emotional-somatic-flashbacks/ - Mentorist — Accessing the Healing Power of the Vagus Nerve (Stanley Rosenberg)
https://www.mentorist.app/books/accessing-the-healing-power-of-the-vagus-nerve/